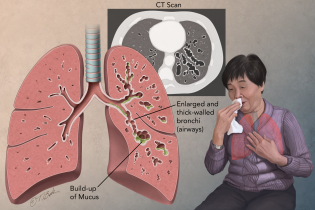
Bronchiectasis in adults
What is bronchiectasis?
— Bronchiectasis is a lung condition that causes a cough (often with mucus), shortness of breath, and other symptoms. In people with this condition, the airways (the branching tubes that carry air within the lungs) are wider than normal. This leads to an increase in mucus, which can be hard to cough up. When mucus stays in the lungs, it makes people with bronchiectasis more likely to get lung infections or bronchitis. Bronchiectasis has many different causes. These include certain infections or problems with the body’s infection-fighting system (called the “immune system”). Other diseases that can cause bronchiectasis include cystic fibrosis and pneumonia.What are the symptoms of bronchiectasis in adults?
— Symptoms of bronchiectasis can include:- A long-lasting cough – The cough usually brings up thick, sticky mucus. It can last weeks or even months.
- Shortness of breath or breathing that sounds like whistling (wheezing).
- Frequent bronchitis or other lung infections.
- A cough that brings up blood – This sometimes happens with bronchiectasis.
- Sharp chest pain – The pain tends to get worse when you take a breath.
Should I see a doctor or nurse?
— Yes. Call your doctor or nurse if:- You are coughing more than usual or your cough bothers you during sleep or other activities
- You have shortness of breath or noisy breathing (wheezing)
- You have new chest pain
- You cough up dark yellow or green mucus, or thick, sticky mucus every day
- You cough up blood
- You have a fever
Will I need tests?
— Your doctor or nurse will learn about your symptoms and do an exam. You might have some or all of these tests:- Blood tests – These can help find the cause of the bronchiectasis, if it is not already known.
- Tests on a sample of mucus you cough up (called a “sputum culture”)
- Chest X-ray
- CT scan of your chest – A CT scan is an imaging test that creates pictures of the inside of the body. It can show a detailed picture of your lungs and airways. A CT scan is usually needed to know if you have bronchiectasis, and to see which parts of the lungs are involved.
- Tests to learn how well your lungs are working (“pulmonary function tests”)
- A test called a “bronchoscopy” – You might have this test if you are coughing up blood. During this procedure, a doctor uses a thin tube (called a “bronchoscope”) to look at the airways inside the lungs.
How is bronchiectasis in adults treated?
— Doctors can give several different treatments to help with symptoms and prevent further problems. These can include:- Medicines to treat and prevent lung infections, reduce airway inflammation, and help thin out mucus in the lungs.
- Airway clearance therapy – This involves loosening the mucus in the lungs so you can cough it up more easily. It is sometimes called “chest physiotherapy.” There is more than 1 way to do this. A doctor, nurse, or therapist can show you the different ways.
- Treatment to stop bleeding in the airways – Coughing up a lot of blood can be life threatening. Doctors can do a procedure called “bronchial artery embolization” to help stop the bleeding. During this procedure, the doctor puts a thin tube into an artery in the leg and moves it up to the lungs. Then he or she uses tiny tools to block the artery in the bleeding area.
- Pulmonary rehabilitation – This is called “pulmonary rehab” for short. In pulmonary rehab, you can learn about other ways to improve your symptoms. This includes getting information about your lung disease, learning ways to save energy, and exercising with a therapist.
- Surgery – If part of a lung is damaged or keeps getting infected, doctors might do surgery to remove the most involved areas.
- Lung transplant – This is done at a transplantation center. A surgeon replaces a person’s diseased lungs with healthy lungs. A lung transplant is done only in people who have severe disease and meet certain conditions.